Summary:
- High levels of lipoprotein(a), or Lp(a), may be associated with a higher risk of heart attack or other serious heart-related events.
- African Americans have higher average Lp(a) levels and are more likely to have heart disease than non-Hispanic whites, but there is not enough information on Lp(a) and cardiovascular disease risk in this population.
- Amgen is sponsoring the African American Heart Study to investigate the association of high Lp(a) levels and atherosclerotic cardiovascular disease (ASCVD)
- deCODE genetics, an Amgen subsidiary, will study the genetic and protein marker information of 5,000 African Americans from across the U.S.
- The unique study also aims to minimize barriers to clinical trial access.
Cardiovascular disease is the number one killer of all Americans. Yet, African Americans are 30% more likely to die from heart disease than non-Hispanic whites.
Having high levels of low-density lipoprotein, or LDL (what some call "bad cholesterol"), is a well-known risk factor for cardiovascular disease, but a less-known risk may involve high levels of a particle called lipoprotein(a), also known as "Lp little a."
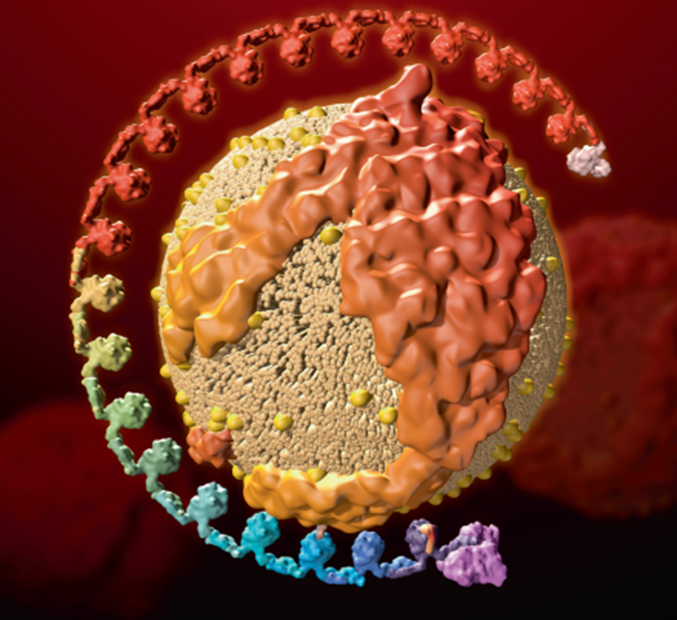
Lp(a) is made up of an LDL particle with a protein called apolipoprotein(a), or apo(a), attached to it. Its size varies depending on the version of the LPA gene that makes the apo(a). Lp(a) is stickier than other types of cholesterol, which may be why high levels are more likely to block arteries and increase risk for heart disease, stroke and other serious heart-related conditions.
Lipoprotein(a) is made up of an LDL particle with a protein called apolipoprotein(a) attached to it.
Up to 20% or over 1.4 billion people worldwide have high levels of Lp(a), which is associated with a person's risk of experiencing a heart attack or other serious cardiac event.
Lp(a) is reported to be an independent risk factor for cardiovascular disease, meaning having high levels of Lp(a) may put people at higher risk, regardless of other cardiovascular risks such as age or high LDL levels. Levels of Lp(a) are also predominantly genetically determined, specifically by which version of the LPA gene an individual inherits. This means if someone has high levels of Lp(a), relatives could be at risk of high levels as well. It also means that lifestyle changes such as diet and exercise will not change levels of Lp(a), though these interventions may still help to reduce the overall risk of heart disease. Even LDL-lowering drugs such as statins do not reduce Lp(a) levels. But thanks to new research, there are investigational treatments being developed that may help those with high Lp(a) levels.
8 Things to Know About Lipoprotein(a)
Why can heart attacks strike people who appear to be perfectly healthy? In some cases, the answer is a little-known risk, lipoprotein(a), which is rarely considered until its impact is felt. Here are 8 things to know about this quiet threat.
LEARN MORE ABOUT Lp(a)
A unique study in an underserved population
On average, African Americans have higher Lp(a) levels than non-Hispanic whites. But most studies of Lp(a) and cardiovascular disease have been done in European populations. To understand the association of high Lp(a) levels with cardiovascular disease in African Americans, Amgen is sponsoring the African American Heart Study.
In partnership with the Association of Black Cardiologists (ABC) and Morehouse School of Medicine in Atlanta, the study aims to recruit 5,000 African Americans—2,500 with atherosclerotic cardiovascular disease (ASCVD), a condition that causes arteries to narrow, blocking blood flow to the heart and brain which can lead to heart attack or stroke, and 2,500 without ASCVD.
The study will benefit from the unique capabilities that ABC and Morehouse School of Medicine, formerly part of the historically Black Morehouse College, bring to the table: reaching Black or African American communities through grassroots engagement, outreach and partnerships with trusted community organizations (churches, barbershops), people (pastors), as well as trial site networks. Many smaller, community-based healthcare practices often don't have the resources to participate in large studies like this one. Participants may also find it challenging to travel to large research sites. This study will address these types of barriers to participation by partnering with these healthcare practices and the patients they serve.
"What has worked in recruiting African American populations to studies is speaking to them through their community leaders," said Dr. Adefisayo Oduwole, M.D., FACC, a cardiologist at Morehouse School of Medicine and ABC member, who is involved with the study. "Going to churches and barbershops to talk with people, doing health fairs, going to doctors' offices, where we answer questions, helps with recruitment." Dr. Oduwole added that when patients see people who look like them running the study, they tend to be more interested in participating.
"We have a significant partnership with healthcare practices that are either members of the Association of Black Cardiologists or affiliated organizations that are focused on the health of African American patients," said Dr. Elizabeth Ofili, M.D., M.P.H., FACC, a cardiologist at Morehouse School of Medicine, who will be helping with recruitment for the study. "By doing this study in the community, we are ensuring that we have a model that could be sustainable in the future."
The study will collect clinical and molecular information, including data on genetic sequencing and protein markers in the blood, and follow participants for at least three years. This information will be analyzed by deCODE genetics, an Amgen subsidiary. The analyses will help researchers and clinicians better understand how genetics and proteins affect the development and progression of ASCVD in African Americans.
Ensuring diversity in clinical research
In 2020, Amgen made a commitment to improve the representation of diverse patients in the company's clinical trials. To do this, the company established the Representation In Clinical ReSEarch (RISE) team that is focused on increasing clinical trial diversity and proportional representation. The team seeks to address the systemic issues that deter people from participating in research, especially those who have been historically excluded due to race, ethnicity, gender, age and other factors. The initiation of the African American Heart Study is a key component of how Amgen plans to deliver on the RISE team's strategic objectives.
"Increasing the diversity in our clinical trials is essential to achieving our ambition of serving all patients. This requires us to think differently than we have in the past about how we design and conduct our trials," said Rob Lenz, M.D., Ph.D., senior vice president of Global Development at Amgen. "To do that, we are educating the community on why this is critical and building trusted relationships with our partners. We also are training external investigators and building new capabilities that will help provide them with the right infrastructures in communities of underserved patient populations to make projects like the African American Heart Study possible."
"There have been systemic barriers for certain populations who may not want to get involved in clinical trials for many reasons," said Ponda Motsepe-Ditshego, vice president and therapeutic area head of inflammation for Global Medicine at Amgen and head of RISE. "Some of it is mistrust of the system, some of it is financial, some of it is geographic." To help address this, the RISE team is partnering externally with community members to address these barriers. "The representation in clinical research work that we do is very important to advance the conversation and to ensure that we are making a difference to all patients. It truly takes a village."